CASE REPORT | https://doi.org/10.5005/jp-journals-10013-1371 |
Rhinosporidiosis: A Surgeon’s Nightmare
1–3Department of ENT, Dr KC Kasliwal’s ENT Centre, Jaipur, Rajasthan, India
Corresponding Author: Anirudh Kasliwal, Department of ENT, Dr KC Kasliwal’s ENT Centre, Jaipur, Rajasthan, India, Phone: +91 9764150028, e-mail: kasliwalanirudh@rediffmail.com
How to cite this article Kasliwal N, Kasliwal A, Kasliwal A. Rhinosporidiosis: A Surgeon’s Nightmare. Clin Rhinol An Int J 2020;13(1):24–26.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Aim and objective: To assess the role of the coblation method in excision of nasal rhinosporidiosis.
Background: Rhinosporidiosis is a granulomatous disease caused by Rhinosporidium seeberi. The most common areas affected are nasal mucosa, ocular conjunctiva, and other mucosae with high chances of recurrence. Among these, the most common area affected is nasal mucosa.
Case description: We present you a case of a 55-year-old man with recurrent nasal rhinosporidiosis, operated 6 times earlier, with recurrence every time within a span of 2–3 months. The patient was then operated on by coblation method and was followed up for 1 year, postoperatively. No recurrence was seen in any follow-up.
Conclusion: Coblation technology is a novel and better technique for the excision of rhinosporidiosis with fewer chances of recurrence.
Clinical significance: The use of coblation for the excision of rhinosporidiosis is a better technique than other methods as it causes less thermal damage to surrounding tissue and less bleeding, prevents spillage to adjacent mucosa, and therefore fewer chances of recurrence.
Keywords: Coblation, Endoscopic surgery, Rhinosporidiosis..
BACKGROUND
Rhinosporidiosis is an uncommon chronic granulomatous infection that affects the nasal mucosa, ocular conjunctiva, and other mucosae. The causal agent is Rhinosporidium seeberi which forms characteristic abundant, large thick-walled sporangium-like structures containing a large number of endospores.1
The disease is most commonly seen in southern India and Sri Lanka, but sporadic cases have been reported from East Africa, Central and South America, Southeast Asia, and other parts of the world.2
The nose is the commonest site of rhinosporidiosis. The fungus causes the production of large sessile or pedunculated lesions that affect one or both nostrils. Nasal rhinosporidiosis infection is insidious in onset and the patient remains unaware of its existence till the patient develops obstruction. The lesions are pink, red, or purple in color and in most cases, the general health of the patient is not affected. The confirmatory diagnosis is by histopathological examination of tissue sections which reveal large, round, or oval sporangia up to 30 μm in diameter. The largest sporangia are filled with spores.3
We present to you a case of recurrent rhinosporidiosis who came to our center with complaints of nasal blockage and recurrent epistaxis. The patient had been operated on six times earlier at different centers but with recurrence every time within a frame of 2–3 months. Coblation-assisted excision of rhinosporidiosis was performed on the patient and postoperative evaluation was done for up to 1 year. No signs of any recurrence were seen.
CASE DESCRIPTION
A 55-year-old male patient came to our center with complaints of nasal blockage and recurrent epistaxis. The patient was a Hindu, living in Rajasthan. He had a history of uncontrolled diabetes mellitus.
On examination polypoidal, a fleshy and reddish mass was seen in the left nasal cavity extending up to the right nasal cavity. Septal perforation was also seen in the cartilaginous part of the septum. On further evaluation of the nasopharynx, oropharynx, eyes, and other mucosal tissues, no mass or growth was seen. The patient was also subjected to a thorough ear nose and throat examination.
Under local anesthesia with 10% lignocaine local spray, he was subjected to flexible-nasopharyngolaryngoscopy which depicted a nasal mass arising from the left nasal cavity and lateral wall of the nose and via the septal perforation, the mass was involving the right nasal cavity (Fig. 1). No growth or mass was seen in the nasopharynx. No growth or mass was seen in the larynx.

Fig. 1: Endoscopic image of nasal mass
Under proper aseptic conditions, the patient was taken up for coblation-assisted excision of rhinosporidiosis under general anesthesia. Intraoperative findings revealed a polypoidal nasal mass arising in the left nasal cavity and lateral wall of the left nostril and extending up to the right nasal cavity. Complete excision of the mass was done and the base was ablated. EVAC 70 and Procise Xp coblation wands were used during the surgery (Fig. 2). The mass was then sent for histopathological examination.
Postoperatively, the patient was started on Tab. dapsone (100 mg) once a day and Tab. doxycycline.
The histopathological report suggested rhinosporidiosis. He was kept on Tab. dapsone (100 mg) once a day for a year. The patient was regularly followed for up to 1 year with endoscopic examination done on 1st month (Fig. 3), 6 months (Fig. 4), and 1 year (Fig. 5) postoperatively. There were no signs of recurrence in any of the follow-up.
DISCUSSION
Rhinosporidiosis is a condition that was initially described by Seeber in 1900, an individual from Argentina.4
The etiologic agent, R. seeberi, has never been successfully propagated in vitro. Initially thought to be a parasite, for >50 years R. seeberi had been considered to be a water mold.5
Molecular biological techniques have more recently demonstrated this organism to be an aquatic protistan parasite, and it has been placed into a new class, the Mesomycetozoea, along with organisms that cause similar infections in amphibians and fish.6
The term coblation is derived from “Controlled ablation”.
The procedure involves a non-heat driven process of soft tissue dissolution using bipolar radiofrequency energy under a conductive medium like normal saline. When current from the radiofrequency probe passes through a saline medium, it breaks saline into sodium and chloride ions. These highly energized ions form a plasma field that is sufficiently strong to break organic molecular bonds within soft tissue causing its dissolution.
Coblation has been recently used frequently to treat various conditions of otorhinolaryngology. The use of coblation in the excision of rhinosporidiosis has not been widely used till now and is a novel technique.
In a study conducted by Nichlani et al., the lesion was excised using a diode laser with a follow-up of 1 year. No recurrence was seen in the patient.7
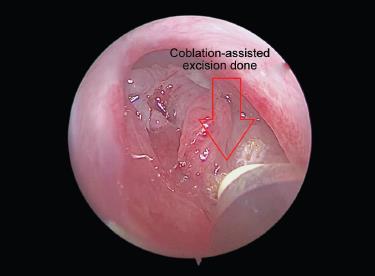
Fig. 2: Coblation-assisted excision of mass

Fig. 3: Postoperative image of nasal cavity after 1 month
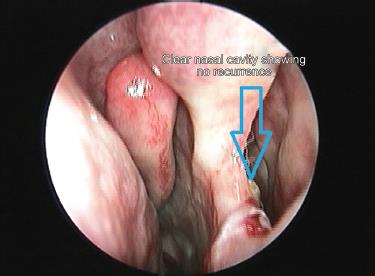
Fig. 4: Postoperative image of nasal cavity after 6 months

Fig. 5: Postoperative image after 1 year
CONCLUSION
Coblation is a newer and better technique in the excision of rhinosporidiosis. As it is done at a temperature of around 60°C, which is far less than the other methods like laser, chances of thermal damage decrease with minimal bleeding intraoperatively and therefore fewer chances of contamination and recurrence.
CLINICAL SIGNIFICANCE
Rhinosporidiosis if not treated early and with the right technique, is a very difficult disease to treat because of its high susceptibility to recurrence and its tendency to spread to the adjacent areas. The coblation method is a newer and alternate method to excise the polyps in rhinosporidiosis. Precise cutting and good postoperative results have made this technique one of the most emerging techniques for the treatment of rhinosporidiosis, for nasopharyngeal, oropharyngeal, and laryngeal masses.
COMPLIANCE WITH ETHICAL STANDARDS
Informed Consent
Informed consent was obtained.
Ethical Approval
All procedures performed involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
REFERENCES
1. Morgan J, Fungi WD, Gleeson A. Scott-Brown’s Otorhinolaryngology, Head and Neck Surgery. 7th ed., Great Britain 2008. p.215.
2. Arsecularatane SN, Ajello A. Rhinosporidium seeberi. ed. L, Ajello RJ, Hay ed. Microbiology and Microbial Infections, vol.4, London: Arnold; 1998. pp.66–73.
3. Morgan J, Fungi WD, Gleeson A. Scott-Brown’s Otorhinolaryngology, Head and Neck Surgery. 7th ed., Great Britain 2008. p.216.
4. Seeber GR. Un neuvo esporozoario parasito Del hombre: dos casos encontrades en polipos nasales. Thesis, Universidad Nacional de Buenos Aires. 1900.
5. Ashworth JH. On Rhinosporidium seeberi (Wernicke 1903) with special reference to its sporulation and affinities. Trans R Soc Edinburgh 1923;53(2):301–342. DOI: 10.1017/S008045680000404X.
6. Fredricks DN, Jolley JA, Lepp PW, et al. Rhinosporidium seeberi: a human pathogen from a novel group of aquatic protistan parasites. Emerg Infect Dis 2000;6(3):273–282. DOI: 10.3201/eid0603.000307.
7. Nichlani S, Jagade MV, Ganeshan AP, et al. Endoscopic resection of nasal rhinosporidiosis with diode laser. Bombay Hospital J 2011;53(1):96–98.
________________________
© The Author(s). 2020 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.